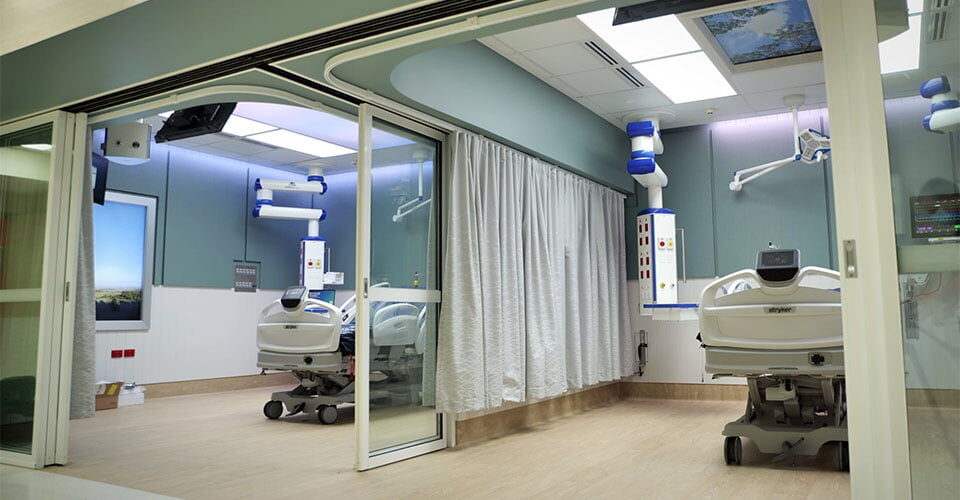
The revolutionary ICU of The Future has been unveiled at The Prince Charles Hospital in Brisbane.
This project, with the potential to change the design of Intensive Care Units all around the world, has come to fruition thanks to the dedication and support of many. The project was led by the Critical Care Research Group (CCRG) with support from The Common Good (an initiative of The Prince Charles Hospital Foundation) and ensured that ICU patients were always at the core.
Patients who had themselves experienced ICU were an integral part of the redesign as they shared their stories with the researchers and others involved in the design and construction of the spaces, so they could better understand the stressors which impact patients during an ICU stay.
Patients like Rebecca Craven.
About Rebecca Craven’s ICU Experience
At age 23, Rebecca Craven was diagnosed with viral cardiomyopathy. Her heart failed, so she began taking medication, but that medication stopped working faster than expected.
Rebecca was placed on the transplant list, but as she faced a lengthy wait, her chances of surviving the wait were low and the decision was made for Rebecca to receive a mechanical heart. Her initial ICU stay for the mechanical heart was for two months, with a further lengthy ICU stay taking place in the months after receiving her heart transplant.
While Rebecca sings the praises of the medical teams who kept her alive and cared for her during this incredibly difficult time, she described her experience in the ICU as traumatic.
“You’re awake the whole time. I think people think that ICU is for critical patients who are asleep and not really understanding what’s going on around them, but for me, I was awake, so I could see everything that was happening around me. I could hear all the beeping noises, I could hear patients in other rooms, you know, when something was happening with them, alarms going off… It was very, very traumatic for me,” Rebecca Craven said.
Rebecca is one of many patients to experience delirium during their stay in the ICU. “You start seeing things and hearing things and it’s quite scary. You think people around you are trying to hurt you. The bed, to me, was sinking in… I thought I was being eaten by the bed. Lots of scary things were happening around me and it was every day,” she said.
Six years have passed since her ICU stay, but the memories of that experience haunt and unsettle her even to this day.
Stressors Addressed by ICU of The Future
Unfortunately, Rebecca’s story is not uncommon, and it is experiences like hers that inspired a group of senior clinicians from CCRG to improve the ICU environment and design; so patients now and into the future can thrive – not just survive.
“Outcomes in intensive care in Australia are fantastic… but we realised more and more as we started to delve into it that people were surviving but that they weren’t thriving. They were going home, they were having terrible nightmares, and terrible hallucinations, they were not getting back to work, and they were left with incapacity. We realised the severe impact of delirium – reversible brain failure,” said Professor John Fraser, CCRG Founder and Director.
“Patients commonly leave ICU with multiple problems they didn’t have before their ICU admission. For example, if you’ve had delirium in intensive care, your risk of developing PTSD is higher than that of a Vietnam Veteran. One-third of former ICU patients still report sleeping difficulty six months later.”
The team involved in the ICU of the Future project, including CCRG Founder and Director Professor John Fraser, Project Manager Oystein Tronstad and psychiatrist Associate Professor Dylan Flaws, realised several factors impacted the brain’s function – particularly the environment.
Their aim was to redesign the ICU environment to optimise healing and recovery while ensuring clinical efficiencies remain at the highest standard.
“The environment is like medicine – a dose of the environment, a dose of anti-biotics, a dose of light. We know that different types of light switch on and off our brain, too much noise is bad for you. So, we realised that when people are at their sickest, too much noise is a little bit like stimulating their brain like making someone with a broken leg run around. It doesn’t allow it to recover. So, we sat back and said let’s start right from ground zero, look at it from the patient perspective, and try and give them a better healing environment,” Professor Fraser said.
Noise monitoring conducted as part of the research showed that trying to sleep in a typical ICU bed space during the daytime was like trying to sleep in the middle of a motorway. At night, they found there were 83 times when it was like sleeping beside a lawn mower.
Features of the ICU of The Future
“We’ve come together to create a healing environment, a cocoon of care if you like, where it’s silent, where the lights can go day or night so that your brain goes day or night, rather than the continuous 24-hour period with no end for a month – which must be torture,” Professor Fraser said.
Some of the most significant innovations in the two new ICU bed spaces at The Prince Charles Hospital include:
- Digital windows to encourage rest and recovery
- Lighting to support circadian rhythm
- Architecturally designed to feel less clinical
- Anti-infection acoustic panels to absorb noise
- State-of-the-art beds for improved comfort and connectivity
- Silent alarms to minimise audible pollution
- Equipment reconfigured to be less distracting and support clinical efficiencies

ICU of The Future Unveiled
On Wednesday, December 14, 2022, the ICU of the Future reached an historical milestone five years in the making, with two new bed spaces unveiled at The Prince Charles Hospital in Brisbane.
Project donors, past ICU patients and their loved ones, ICU staff members, and researchers who have been working for years to incorporate the right design elements to address patient stressors, came together to mark this historic milestone.

Rebecca was one of several patients consulted during the design process, and their input was invaluable. She stepped inside the new bed spaces on Wednesday and described them as “amazing”.
“In the hospital, all you want to do is be at home, but I think this new ICU is exactly what’s needed. It’s more homey to me, and that’s something that feels comfortable when you’re a patient when you’re trying to recover from a major surgery,” Rebecca said.

The collaborative project has seen Metro North Health, CCRG and The Common Good join forces along with a range of other parties.
“We had to build a team of former patients and their family members, and clinicians and researchers with relevant experience from ICU. There were also a lot of external partners because we could not have solved all these problems without talking to the right people – so IT companies, architects, designers, builders, tech companies,” Project Manager Oystein Tronstad said.
Delivering a project of this magnitude relies on many people coming together for the common good. Over the past three years, The Common Good rallied the support of the community, with over 900 incredible and generous supporters answering the call for help and making a donation to this life-changing project.
“Doing innovation in this sort of setting relies on the generosity of mums and dads, and that’s who we turn to. We are incredibly grateful for their support, and they should feel proud of their contribution as it’s those individuals who help make many ground-breaking discoveries, like this one, possible,” Michael Hornby OAM, The Common Good CEO, said.
“We are incredibly grateful for people who’ve contributed their time, their expertise and given money to this project. Without their support, this wouldn’t have happened, and we would have had to stop many years ago,” Oystein Tronstad said.
Testing the Success of the ICU of The Future
The opening of these two bed spaces has marked an incredible, historic milestone; however, there is plenty more work to be done with patients due to be admitted in early January 2023.
“Now the real work starts. We start to analyse people’s sleep waves, we start to analyse their stress hormones, we start to analyse how well they can mobilise, we start to look at post-intensive care syndrome to see to how they cope,” Professor Fraser said.
“We’re hoping this project will benefit future ICU patients, not just at this hospital but at all hospitals – locally, state-wide, nationally, and internationally,” Oystein Tronstad said.

To learn more about the ICU of the Future project, click here.