Growing skin cells may be one solution to helping battle cardiovascular disease.
Cardiovascular disease is the number one cause of death globally and there aren’t enough donor hearts to match the ever-increasing need. Thankfully with decades of incredible research and hard work, doctors and researchers have been able to develop the ventricular assist device (VAD), a type of artificial heart that helps to pump blood cells around the body when the natural heart fails.
These life-saving devices do come with their shortfalls though and there is constant work being undertaken to improve and perfect them for better patient outcomes. One common complication’s infection, which often starts at the driveline – a cable which connects the internal VAD with an externally placed battery. While one direction of research is to remove the need for these drivelines altogether, realistically this work won’t be in use for potentially a decade.
In the meantime, researchers at The Prince Charles Hospital, Dr Shaun Gregory and Eleonore Bolle, have teamed up with QUT researchers Dr Tim Dargaville and Dr Tony Parker, to take a different approach; testing infection-resistant materials to use on the driveline. In addition to trying a new array of materials that reduce the chance of infection, the team are also looking into ways to do something never done before in this field-create a 3D printed mesh that tissue can grow on.
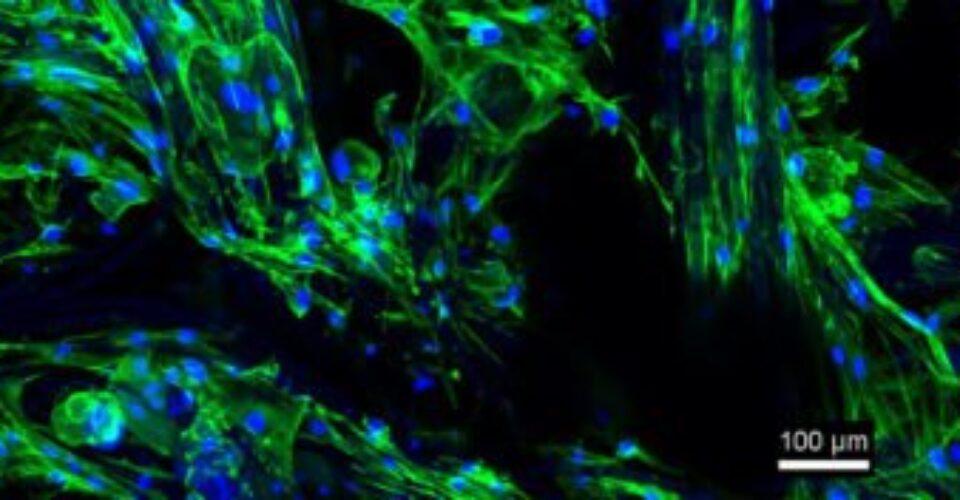
“I used small pieces of both materials [polyurethane and Dacron] and placed skin cells on them , and then monitored them for 7 days. While cells formed a uniform layer on the polyurethane, they infiltrated the Dacron samples and wrapped around the fibres,” explained Eleonore. The results of this can be seen in the picture below.
Watch this space to hear more exciting news about this project in the future!
Support The Common Good here.